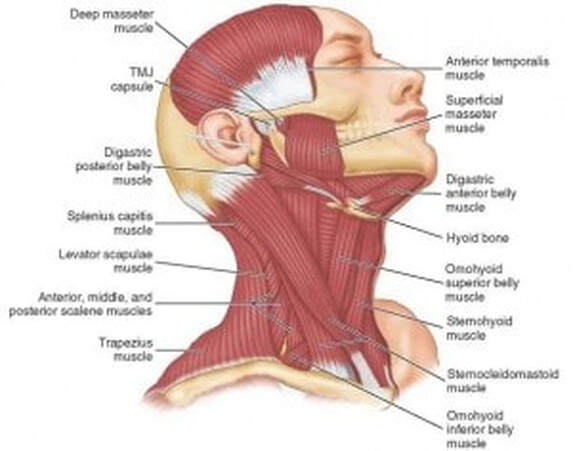
 Have you been experiencing frequent headaches, back and neck pain, dull aching facial pain, or popping in your jaw? You are not alone, many of my clients walk through the door experiencing the very same. Many of these symptoms may be related to a Temporomandibular Disorder (TMD). These disorders involve the jaw muscles and/or the jaw joint known as the Temporomandibular Joint (TMJ). The TMJ is the hinge that connects your jaw to the bones on the side of your skull, which are in front of each ear. Below are a few causes of trauma to the TMJ: * Direct trauma * Indirect trauma – whiplash, neck injury * Stress and emotional strain * Poor posture * Clenching/grinding of teeth * Myofascial restrictions throughout the body * Rotation in the pelvis * Tooth loss or misalignment of the teeth * Chewing gum or biting nails Taking a global approach to the tension often found within the joint can help relieve symptoms and alleviate causes that are not related to TMD. Within the clinic, I approach the jaw joint pain with a combination of myofascial release (MFR), triggerpoint therapy (TrP), and craniosacral (CST). Releasing the triggerpoints and elongating the connective tissue allow for improved symptoms and giving your body the ability to heal itself. There is not a single cause for TMD symptoms. Clicking or popping noises, locking or grating sensations, pain or stiffness in and around the jaw and TMJ can all be symptoms of TMD. Many also experience headaches, neck pain, or earaches. Other known causes of jaw or facial pain include conditions, such as:
TMD, like many other symptomatic complexes, can often have several different factors that contribute to its development. If you suffer from jaw, head or neck problems and would like to learn ways to help release tension, check out our new Client Resources page. I have uploaded a pdf with techniques to help you manage symptoms at home.  There is soooo much confusion about this issue. It’s a shame because therapeutic icing and heating — cryotherapy and thermotherapy — are rational, cheap, easy, safe self-treatment options for many common painful problems. Ice and Heat, the Basics! Ice is for fresh injuries, and heat is for stiff, aching muscles. Roughly. But the devil is in the details, and there are a lot of them. Ice is for injuries and inflammation— calming down damaged superficial tissues that are inflamed, red, hot and swollen. The inflammatory process is a healthy, normal, natural process … that also happens to be incredibly painful and more biologically stubborn than it needs to be. Icing is mostly just a mild, drugless way of dulling the pain of inflammation and taking swelling down a bit … we hope. Examples: a freshly pulled muscle or a new case of IT band syndrome (which is more likely to respond than the other kind of runner’s knee, patellofemoral pain, because ITBS is superficial and PFPS is often a problem with deeper tissues). Heat is for muscles, chronic pain, and stress — taking the edge off symptoms like muscle aching and stiffness, which have many unclear causes, but trigger points are probably one of the usual suspects. Chronic pain, especially back pain, often involves lots of tension, anxiety, hypervigilance, and sensitization, and comfortable heat can soothe a jangled mind and nervous system. Alternating between applications of ice and heat is called contrasting therapy. It’s extremely stimulating and is mostly used to facilitate injury recovery, with unknown efficacy. Ice and Heat, be CAREFUL: Both ice and heat have the potential to do some minor, temporary harm when used poorly. Heat can make inflammation significantly worse. Ice can aggravate symptoms of tightness and stiffness. Both ice and heat are pointless or worse when unwanted: icing when you’re already shivering, or heating when you’re already sweating. The brain may interpret an excess of either one as a threat. If you add heat to a fresh injury, watch out: it’s going to get worse! Heat and inflammation are the other particularly bad combination. If you add heat to a fresh injury, watch out: it’s going to get worse! A physician once told my father to heat a freshly injured knee, and wow — it swelled up like a balloon, three times bigger than it had been before. And three times more painful. I have seen clients, way too often, put heat on their neck/shoulder after waking up with pain and create even more pain and their necks seize up and become more immobile. What about injured muscle? Muscle strains? If you’re supposed to ice injuries, but not muscle pain, then what do you with injured muscles (a muscle tear or muscle strain)? That can be a tough call, but ice usually wins — but only for the first few days at most, and only if it really is a true muscle injury. A true muscle injury usually involves obvious trauma during intense effort, causing severe pain suddenly. If the muscle is truly torn, then use ice to take the edge off the inflammation. Is ice better than heat? Is heat better than ice? Ideal uses of ice and heat are roughly equal in potency — which isn’t very potent. Neither is strong medicine. The reason to use them is not that they are highly effective treatments — they rarely are — but because they are so cheap, easy, and mostly safe, especially compared to many other popular treatments. A Word on Low Back Pain Most “strained” backs are not actually damaged — it just feels like it. When people think they’ve “thrown their back out,” there is rarely anything out of place, or nothing that actually hurts. Even if there is — like herniated discs (“slipped” discs) — the problem is much deeper than the limited penetrating power of either ice or heat can reach. So why does it even matter? Why choose either one? Back and neck pain are mysterious and hard to explain. As they get chronic, they get even more mysterious. This weirdness is probably because they are often about neurological over-reaction to relatively minor or stale threats. Our nervous systems are paranoid about potential spinal hazards, and the bark (pain) is usually worse than the “bite” (actual tissue trouble). Pain will dial up or down in proportion to how “worried” our brains are about the situation. This is “The Mind Game in Low Back Pain.” So, be mindful. Ice can dial up neurological sensitivity, but heat can relax muscle to create more instability and pain. Here’s a checklist.
A Word on Stretching I always recommend icing before/after intense stretching. Why? Simply put, stretching does cause minor tissue damage and inflammation. When working with my pro athletes we are working on either opening up the joints or lengthening tissue. Lengthening tissue is very calculated and my athletes are cold when we start and I throw them in a cryo chamber or ice when we are done to decrease the inflammation and stimulate lymphatic and blood flow. If you decide you need calculated, intense stretching please give me a call or email so we can talk and prepare your body for recovery. The bottom line The bottom line is: use whatever feels best to you! Your own preference is the tie-breaker and probably the most important consideration. For instance, heat cannot help if you already feel unpleasantly flushed and don’t want to be heated. And ice is unlikely to be effective if you have a chill and hate the idea of being iced! If you start to use one and you don’t like the feel of it … just switch to the other. Article by Lisa McNeil and Paul Ingraham
|
AuthorSA little from Dr. Dan, a little from Lisa but always a lot of good stuff! Archives
January 2024
Categories
All
Or
|
Your Orthopedic Wellness Clinic
Located at:
285 N Janacek Rd, Suite C
BROOKFIELD, WI
285 N Janacek Rd, Suite C
BROOKFIELD, WI
HOME TO APPROVED THERAPIST FOR:
©2022 MOMENTUM MOVEMENT CLINIC

 RSS Feed
RSS Feed





